What is the Retina?
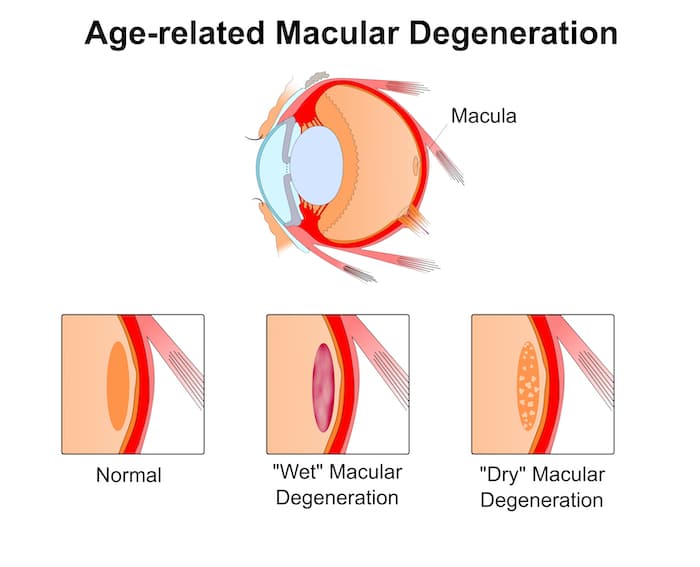
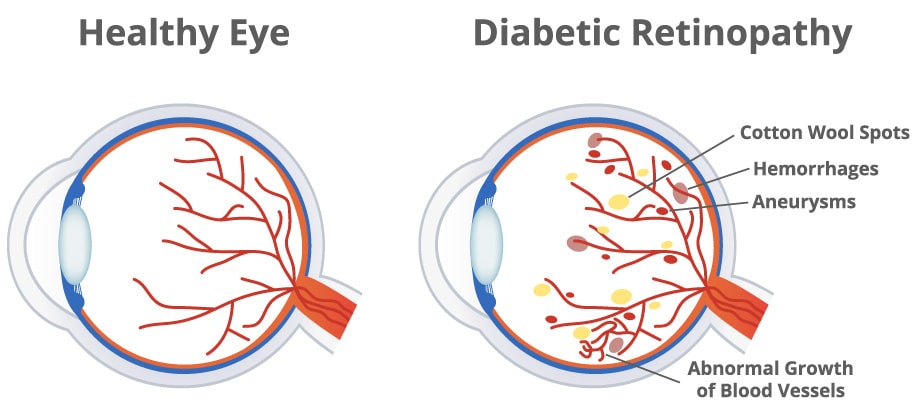
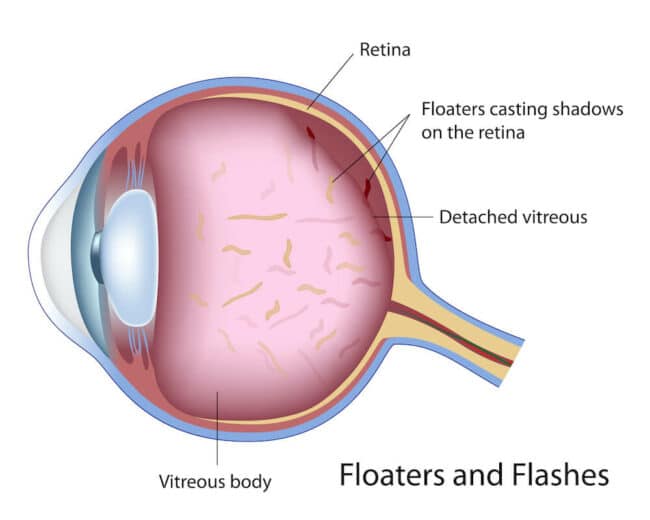
The retina is a thin layer of light-sensitive tissue at the back of the eye that plays a vital role as it contains millions of specialized cells that detect light and color, enabling us to perceive detail and depth. Damage to the retina can lead to vision impairment or blindness, so retinal health is crucial for maintaining clear and functional sight.
At Aker Kasten Eye Center, we provide comprehensive care for retinal conditions, helping preserve your vision and improve eye health.